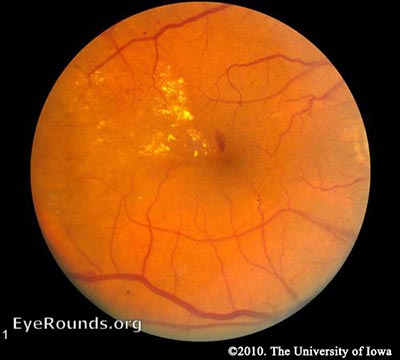
Biomarkers may facilitate a better understanding of diabetic retinopathy, and contribute to the development of novel treatments and new clinical strategies to prevent vision loss in people with diabetes. Given the increasing incidence and prevalence of diabetes, and the limited capacity of healthcare systems to screen and treat diabetic retinopathy, there is need to reliably identify and triage people with diabetes. New analytical techniques, in particular those related to molecular markers, are accelerating progress in diabetic retinopathy research. Therefore, more effective treatments for diabetic retinopathy are necessary. Unfortunately, in spite of a range of treatments (including laser photocoagulation, intraocular steroids, and anti-VEGF agents, and more recently oral fenofibrate, a PPAR-alpha agonist lipid-lowering drug), many patients with diabetic retinopathy do not respond well to current therapeutics. Greater knowledge of novel biomarkers and mediators of diabetic retinopathy, such as those related to inflammation and angiogenesis, has contributed to the development of additional therapeutics, in particular for late-stage retinopathy, including intra-ocular corticosteroids and intravitreal vascular endothelial growth factor inhibitors ('anti-VEGFs') agents. Common biomarkers of diabetic retinopathy and its risk in clinical practice today relate to the visualization of the retinal vasculature and measures of glycemia, lipids, blood pressure, body weight, smoking, and pregnancy status. Screening for diabetic retinopathy is recommended to facilitate early detection and treatment. There are multiple risk factors and markers for the onset and progression of diabetic retinopathy, yet residual risk remains. Diabetic retinopathy is the most frequently occurring complication of diabetes it is greatly feared by many diabetes patients. Whilst improved diabetes care has substantially improved diabetes outcomes, the disease remains a common cause of working age adult-onset blindness. There is also an as yet unexplained increase in the incidence of type 1 diabetes, which is not related to adiposity. This coincidence may lead to a rise in the prevalence of type 2 diabetes. There is a global diabetes epidemic correlating with an increase in obesity.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
